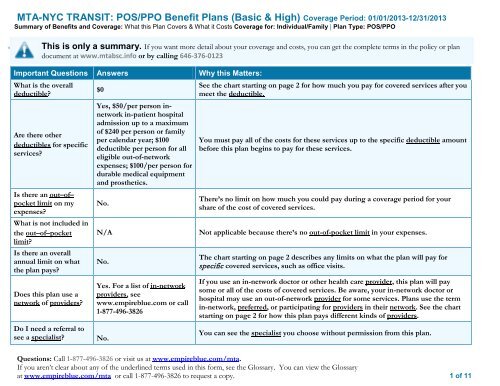 
Visits are typically covered with copayments, and members with original Medicare are assessed a 20 percent copayment with every visit to a mental health care provider. There is no need for policy holders to get a referral for mental health care from their primary care providers if they have coverage under a BCN Advantage plan. Once logged in, policyholders should select Go to My Coverage, and then tap on Medical, select the What’s Covered option, and then click on Find Behavioral Health Care, Mental Health Care and Substance Use Treatment.Īfter accessing the services available for behavioral health and substance abuse services, policyholders can find information regarding plan requirements necessary to obtain services, which services their individual plan offers, how much they must pay for services (such as copays and deductibles) and how much their plans pay for covered services.Ĩ6 Blue Cross Blue Shield Medicare Coverage Policyįor policyholders who have Medicare coverage through Blue Cross Blue Shield, mental health services are covered. This involves accessing the Blue Cross Blue Shield website or its mobile app. Insured policyholders can check on their individual coverage levels by logging into their Blue Cross Blue Shield member accounts. How To Check Blue Cross Blue Shield Insurance Coverage for Mental Health Therapy Check your Blue Cross Blue Shield policy details to determine if you have a deductible and if you must pay a copayment with your mental health services. For instance, your policy may require you to pay a certain percentage of your treatment costs per visit or a set amount per visit or service, such as $40. You may also need to pay a copay for each visit or treatment. 
For example, if your policy has a $500 deductible, then you are responsible for the first $500 in care. With most health insurance plans, including plans from Blue Cross Blue Shield, you must first meet your deductible prior to receiving coverage. Some services available may also include case management services, consultations and outpatient services.īlue Cross Blue Shield Therapy Treatment Deductibles and Copays You will need to choose a mental health provider in the BCBS network in order to be covered. For this reason, it is important to check your individual policy to make sure you’re covered. What’s more, employers have the ability to customize the benefits that they offer, and they can also determine what the insured must do in order to access these benefits. Still, it is important to note that BCBS plans may have stipulations that must be met in order for coverage to be provided. Most network plans from BCBS cover applied behavior analysis, residential treatment, emergency mental health care, group therapy, and other mental health services. 86 Blue Cross Blue Shield Therapy Coverage Services
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
